In recent years, the term “spondylosis” has become more prevalent in medical circles and among individuals dealing with spine health issues. This blog post aims to elaborate on various facets of spondylosis, including its causes, symptoms, diagnosis, and prevention.
Spondylosis of the Spine
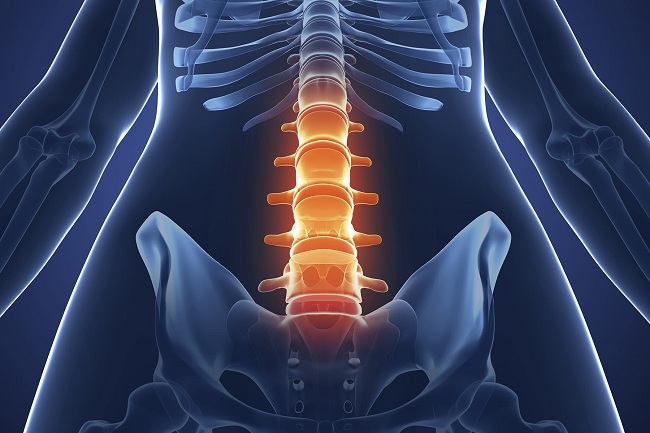
Spondylosis refers to a type of arthritis stemming from wear and tear and aging. It generally affects the spine, leading to the loss of cushioning between the vertebrae which in turn can cause pain and stiffness.
Spondylosis Pathophysiology
The pathophysiology of spondylosis involves the degenerative changes in the spine such as disk degeneration, formation of bone spurs, and a decrease in the height of the vertebral disc. It is a progression that occurs over many years due to age-related wear and tear.
What Causes Spondylosis?
The primary causes of spondylosis include aging, a history of spinal injuries, genetic predisposition, and lifestyles involving heavy lifting or sedentary habits. Moreover, conditions such as congenital spondylosis can be present from birth, further predisposing individuals to this ailment.
Scoliosis and Spondylosis
While scoliosis refers to a sideways curvature of the spine, often diagnosed in childhood or adolescence, it can coexist with spondylosis, exacerbating the degenerative process and complicating the clinical picture with symptoms such as back pain and stiffness.
Spondylosis Deformans
This refers to a severe form of spondylosis characterized by significant deformity of the spine, including abnormal curvature such as kyphosis (a forward rounding of the back) and scoliosis, leading to functional impairments and a reduced quality of life.
Spondylosis Kyphosis
Kyphosis in the context of spondylosis refers to an exaggerated forward rounding of the back, often resulting from vertebral fractures and osteoporosis. It presents a host of challenges including pain, limited mobility, and aesthetic concerns.
Spondylosis Etymology
The term spondylosis is derived from the Greek word “spondylos,” which means vertebra. The nomenclature is aptly chosen to refer to the degenerative changes affecting the vertebral column.
Understanding Diagnosis
Diagnosing spondylosis involves a series of steps including physical examination followed by imaging tests such as X-rays, MRI, and radiology which help in visualizing the structural abnormalities and the extent of degeneration.
Spondylosis Radiology, MRI, and X-ray
These diagnostic tools offer detailed views of the spine. While X-rays give an outline of the spine highlighting bone spurs or narrowing of space between vertebrae, MRI offers a detailed view of the soft tissues including the discs and nerves, aiding in the accurate diagnosis.
Managing and Preventing Spondylosis
Prevention and management strategies for spondylosis include maintaining a healthy lifestyle with regular exercise and a balanced diet to foster spine health.
Spondylosis Sleeping Position and Mattress
Choosing the right mattress is vital in managing spondylosis pain. A medium-firm mattress often offers the best support. Furthermore, sleeping in a neutral position can aid in alleviating symptoms.
Massage for Spondylosis
Therapeutic massages can offer relief by reducing muscle tension and improving mobility. It’s advisable to consult with a healthcare provider for personalized advice.
Conclusion
Understanding spondylosis from various angles — its etymology, pathophysiology, associated conditions like scoliosis and kyphosis, and diagnostic tools such as MRI and radiology — can equip you with the knowledge to manage and prevent this condition effectively. Remember to always consult with a healthcare provider for personalized medical advice.